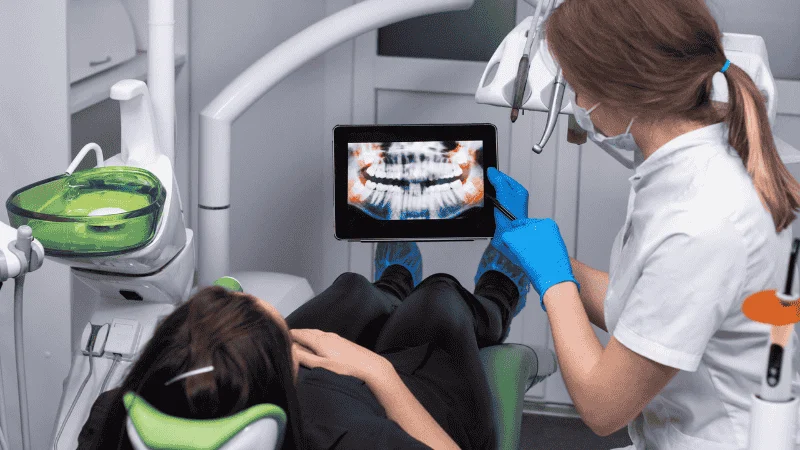
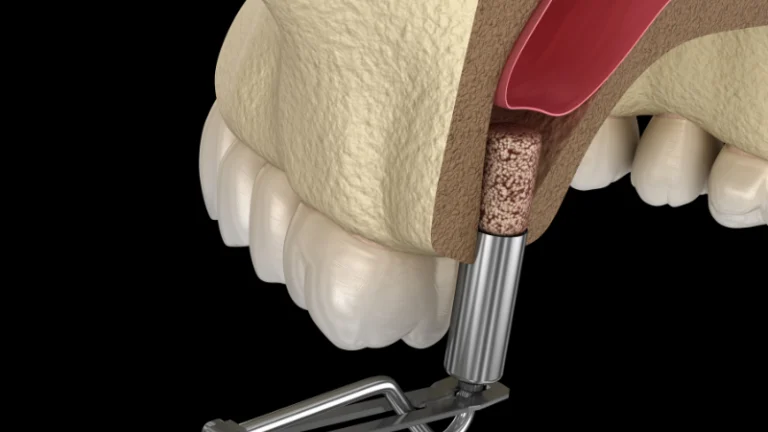
Dental implants offer a lasting solution for missing teeth, but their success depends heavily on the health of your gums. If you’re dealing with gum disease, you might wonder whether it will prevent you from getting implants or affect how well they work.
Gum disease can significantly reduce dental implant success rates by damaging the jawbone and soft tissue that support the implant.
The bacteria from gum disease attack the bone structure needed for the implant to fuse properly with your jaw. Without this solid foundation, the implant can loosen or fail completely.
The good news is that gum disease doesn’t automatically disqualify you from getting dental implants. With proper treatment and careful planning, many patients with gum disease can still achieve high implant success rates.
Understanding how gum disease affects dental implants and what steps you need to take can help protect your investment and ensure a healthy smile for years to come.
Key Takeaways
- Gum disease damages the bone and tissue that dental implants need to stay secure
- Treating gum disease before implant placement greatly improves your chances of success
- Proper care after getting implants prevents new gum problems and protects your investment
Receive advanced gum and implant care across Miami, Pembroke Pines, and Delray Beach, FL.
How Gum Disease Impacts Dental Implant Outcomes
The health of your gums plays a major role in whether your dental implants succeed or fail. Gum disease can seriously impact the stability and lifespan of your implants by affecting the bone and tissue that hold them in place.

Gum Health and Implant Success
Your dental implants need healthy gums and strong bone to stay secure. The process of osseointegration is when your implant fuses with your jawbone. This takes several months and creates a stable base for your replacement tooth.
When you have gum disease, this process gets interrupted. Periodontal disease causes inflammation that weakens the tissues around your implant. The infection can spread to the bone and prevent proper healing.
Patients with a history of periodontal disease have lower dental implant success rates compared to those with healthy gums. Gingivitis is the early stage where your gums become swollen and bleed.
If it progresses to periodontitis, you face more serious problems that threaten your implant.
Risks of Untreated Gum Disease
Leaving gum disease untreated puts your implants at risk in several ways. The infection destroys the supporting bone and tissues that keep your implant stable. This bone loss weakens the foundation your implant depends on.
Key risks include:
- Progressive bone deterioration around the implant site
- Loosening of the implant over time
- Complete implant failure requiring removal
- Infection spreading to nearby teeth and gums
Periodontitis creates pockets of infection between your teeth and gums. These pockets harbor bacteria that attack both natural teeth and implants. The longer the disease goes untreated, the more damage occurs to your jawbone.
Peri-Implantitis: Infection Around Implants
Peri-implantitis is an inflammatory condition that affects the soft and hard tissues surrounding your implant. It’s similar to gum disease but happens specifically around dental implants. This condition is one of the leading causes of implant failure.
The infection causes your gums to pull away from the implant. Your bone begins to deteriorate, and the implant loses its anchor. You might notice bleeding, swelling, or pain around the implant site.
If you had periodontal disease before getting implants, you’re at higher risk for developing peri-implantitis. The same bacteria that caused your original gum disease can attack your implants.
Without treatment, the infection will continue to destroy bone until the implant fails completely.
Visit our clinic to treat gum disease before implant placement.
Dental Implant Eligibility With Gum Disease
Your eligibility for dental implants depends on the severity of your gum disease and the health of your jawbone. Dentists must evaluate both your gum condition and bone density before determining if you can proceed with implant placement.
Assessing Gum and Bone Health
Your dentist will perform a thorough examination to check if you’re a good candidate for dental implants. This assessment includes measuring pocket depths around your teeth, checking for gum inflammation, and evaluating any gum recession.
X-rays and CT scans help determine if periodontitis has caused bone loss in your jaw. The severity of your condition can restrict gum disease implant eligibility, especially if you have advanced periodontal disease or significant bone deterioration.
Your jawbone needs to be strong enough and thick enough to hold the implant securely. If bone loss has occurred, you might not qualify for traditional implants without additional procedures.
Your dentist will also look at your overall health, including conditions like diabetes that can affect healing and implant success rates.
Treating Gum Disease Before Implant Placement
You’ll need to address active gum disease before getting dental implants. For mild cases, your dentist might recommend improved brushing and flossing techniques along with professional deep cleanings to remove bacteria below the gum line.
More severe periodontitis requires treatments like laser gum surgery to reduce pocket depths and help your gums reattach to your teeth. These procedures eliminate infection and create a healthier foundation for implants.
If you’ve experienced bone loss, you’ll likely need a bone graft before implant placement. Bone grafting adds transplanted bone material to build up weak areas of your jaw.
The healing process takes several months as the new bone integrates with your existing bone structure.
While this extends your treatment timeline, it significantly improves your chances of successful implant placement and long-term stability.
Book a consultation to improve dental implant success with proper gum disease treatment.
Treatments for Gum Disease Prior to Implants
Before you can receive dental implants, your gums and bone must be restored to health through proper treatment.
The specific approach depends on how severe your gum disease is, but the goal is always to eliminate infection and create a stable foundation for your implants.
Scaling and Root Planing
This deep cleaning procedure is typically the first treatment your dentist will recommend for moderate gum disease.
During the process, your dental professional removes plaque and tartar buildup from below your gumline where regular brushing can’t reach.
The root planing part smooths the surfaces of your tooth roots. This helps your gums reattach to your teeth more easily.
The procedure usually involves:
- Numbing the treatment area for your comfort
- Cleaning deep pockets between your teeth and gums
- Removing bacterial deposits from root surfaces
- Smoothing rough spots where bacteria tend to gather
You might need multiple visits to complete the treatment depending on how much gum disease you have. Your dentist may also prescribe antibiotics to help control bacterial infection during healing.
Most patients notice less bleeding and swelling within a few weeks after scaling and root planing.
Gum Surgery and Bone Grafting
When gum disease has progressed to an advanced stage, you may need surgical treatment before implants become possible. Flap surgery allows your periodontist to access deep infection areas by temporarily lifting your gum tissue away from your teeth.
Bone loss is a major challenge that often requires bone grafting to rebuild your jaw structure. Without enough bone, dental implants won’t have the support they need to stay stable.
Bone graft materials can come from:
- Your own bone (usually from another part of your jaw)
- Donor bone tissue
- Synthetic bone substitute materials
After a bone graft, you’ll need several months of healing time before implant placement. Your body needs this time to integrate the graft material and form new, strong bone tissue. This waiting period is essential for long-term implant success.
Laser Therapy and Advanced Interventions
Laser therapy offers a less invasive option for treating gum disease in some cases. The laser targets and removes infected tissue while leaving healthy gums intact.
This treatment often causes less bleeding and discomfort than traditional gum surgery. You may experience faster healing times and reduced swelling after the procedure.
Benefits of laser therapy include:
- More precise removal of diseased tissue
- Reduced need for stitches
- Lower risk of infection
- Less post-treatment pain
Some dental practices combine laser therapy with other treatments for better results. Your dentist might also recommend antimicrobial mouth rinses or antibiotic therapy alongside these procedures to control bacteria levels.
The specific combination of treatments you receive will depend on your individual situation and how your gums respond to initial treatment.
Preventing Gum Problems After Dental Implant Placement
Taking care of your gums after getting dental implants protects your investment and keeps your mouth healthy. Good daily habits and regular checkups help you catch problems early and maintain strong, lasting implants.
Oral Hygiene Practices
Brush your teeth twice daily using a soft-bristled toothbrush and non-abrasive toothpaste. Pay special attention to the area where your implant meets your gums, as bacteria can collect there.
Floss at least once every day to remove plaque between your implants and natural teeth. Use floss threaders or interdental brushes designed for implants to clean hard-to-reach spaces. These tools work better than regular floss around implant posts.
Add an antimicrobial mouthwash to your routine to reduce bacteria that cause inflammation. Rinse after brushing and flossing to reach areas your brush might miss. Avoid alcohol-based mouthwashes if they irritate your gums.
Daily habits that protect your implants:
- Brush gently around the implant site
- Clean between teeth with specialized floss or brushes
- Rinse with antimicrobial mouthwash
- Avoid smoking, which increases infection risk
- Limit sugary foods that feed harmful bacteria
Regular Dental Visits
Schedule professional cleanings every six months to remove tartar buildup you can’t eliminate at home. Your dentist uses special tools to clean around implants without damaging them.
Your dentist checks for early signs of peri-implantitis during these visits. They measure the depth of gum pockets around your implants and look for bone loss on X-rays. Deep cleaning may be needed if pockets become too deep or if infection develops.
These appointments help maintain a high implant success rate by catching issues before they become serious. Your dental team can adjust your home care routine based on what they see during exams.
Recognizing Early Signs of Complications
Watch for red, swollen, or tender gums around your implants. Bleeding when brushing or flossing signals inflammation that needs attention.
Bad breath that doesn’t go away with normal brushing could indicate bacterial infection. Pain or discomfort around the implant site is another warning sign you shouldn’t ignore.
Contact your dentist right away if you notice any looseness in your implant. Early treatment prevents minor problems from turning into implant failure.
The sooner you address these symptoms, the better your chances of saving your implant and restoring your oral health.
Managing Gum Disease With Existing Dental Implants
If gum disease develops after you already have dental implants, quick action helps protect your investment. Regular dental visits catch problems early, and proper daily care keeps bacteria under control around your implant sites.
Treating Peri-Implantitis
Peri-implantitis is an infection that affects the gum tissue and bone around your dental implants. It works like gum disease but targets implant sites instead of natural teeth.
Your dentist will first perform scaling and root planing to remove bacteria and tartar from below the gum line. This deep cleaning reaches areas you can’t access with regular brushing. Some cases need antibiotics to fight infection.
More severe peri-implantitis may require surgical treatment. Your dentist might need to:
- Remove infected tissue around the implant
- Clean the implant surface directly
- Add bone grafting material if bone loss occurred
- Use laser therapy to reduce bacteria
The earlier you catch peri-implantitis, the better your chances of saving the implant. Watch for warning signs like bleeding gums, swelling, or discomfort around your implants.
Maintenance for Long-Term Implant Health
Your daily oral hygiene routine matters just as much after getting implants as before. Brush twice daily using a soft-bristled toothbrush and clean around each implant carefully.
Floss or use interdental brushes designed for implants to remove plaque between teeth. Water flossers work well for reaching tight spaces around implant crowns.
Schedule professional cleanings every 3-6 months rather than the standard twice yearly. Your dental team uses special tools that won’t scratch implant surfaces while removing buildup.
Avoid smoking completely. Tobacco use dramatically increases your risk of implant failure and makes gum disease harder to control.
Tell your dentist right away if you notice any changes around your implants, including redness, bleeding, or loose feeling restorations.
Alternatives to Dental Implants for Severe Gum Disease
When gum disease has caused significant bone loss or damage, other tooth replacement options may work better than implants. Dentures offer a proven solution that doesn’t require the same level of bone support.
When Dentures May Be Recommended
Your dentist may suggest dentures if you have severe periodontal disease that has weakened your jawbone too much for implants. Dental bridges, partial dentures, and full dentures can all provide effective alternatives when bone loss is extensive.
Partial dentures work well when you still have some healthy teeth remaining. They attach to your natural teeth and fill in the gaps left by missing teeth. Full dentures replace all your teeth in the upper or lower jaw.
Implant-supported dentures offer a middle option if you have enough bone in certain areas. These dentures snap onto a few strategically placed implants where your jawbone is strongest.
This gives you more stability than regular dentures without needing implants for every missing tooth.
Your dentist will examine your gums and take imaging scans to determine which option fits your situation best. The right choice depends on how much bone you have left and how well you can manage your gum disease going forward.
Frequently Asked Questions
Active gum disease creates risks for implant placement, but treatment can restore your candidacy. Understanding warning signs and maintenance requirements helps protect your investment in dental implants.
Is it safe to get dental implants with active gum disease?
Getting dental implants with active gum disease is not recommended. The bacterial infection that causes gum disease can spread to your implant and prevent proper healing.
Your dentist needs to treat the gum disease first before moving forward with implant surgery. Active gum disease lowers the success rates of dental implants by eroding the jawbone that anchors the implant.
The bacteria from untreated gum disease don’t disappear when teeth are removed. They will continue to multiply and can attack your new implant, leading to complications that are harder to treat than the original gum disease.
How does existing periodontal disease influence the success of a dental implant?
Periodontal disease damages the bone and gum tissue that support your implant. This damage affects a process called osseointegration, where the titanium post fuses with your jawbone.
Without a solid foundation, your implant cannot bind properly to the bone. Failure rates can significantly increase in patients with gum disease due to poor bone structure.
The weakened bone may require additional procedures like bone grafts before implant placement. Your jawbone needs adequate density and health to hold the implant securely in place for many years.
What are the best practices for ensuring dental implant success if I have a history of gum disease?
You need to complete periodontal therapy before getting implants. This treatment removes bacteria and helps your gums heal properly.
Your dentist may recommend scaling and root planing to clean below the gum line. In some cases, you might need gum surgery to address deeper infections or bone loss.
If you smoke, you should stop at least four weeks before and after the procedure. Implants placed in smokers present with a 140% higher risk of failure than implants placed in non-smokers.
Bone grafting might be necessary to rebuild lost bone structure. This extra step creates a stronger foundation for your implant to succeed long-term.
Can treating gum disease improve my chances for a successful dental implant?
Yes, treating gum disease significantly improves your implant success rates. Successfully treating the gum disease restores candidacy and ensures long-term implant stability.
Proper periodontal therapy eliminates the harmful bacteria causing inflammation. This allows your gums and bone to heal and regain strength.
With effective treatment, patients with a history of gum disease can achieve high implant success rates. The key is waiting for your gums to fully heal before proceeding with implant placement.
What signs of gum disease should I look out for before considering a dental implant?
Watch for red, swollen, or bleeding gums when you brush or floss. These are early warning signs that bacteria are infecting your gum tissue.
Receding gums that make your teeth look longer indicate bone and tissue loss. You might also notice persistent bad breath that doesn’t go away with regular brushing.
Loose teeth or changes in how your teeth fit together signal advanced gum disease. Pus between your teeth and gums is another serious sign that requires immediate dental attention.
Pain when chewing or increased tooth sensitivity can indicate gum problems. If you notice any of these symptoms, schedule a dental exam before considering dental implants.
How does ongoing periodontal maintenance play a role in the longevity of dental implants?
Regular periodontal maintenance protects your implant from future infection. You can develop gum disease around an implant even after successful placement.
Professional cleanings remove plaque and tartar that your toothbrush can’t reach. Your dentist will monitor your gums and bone levels to catch problems early.
Daily brushing and flossing remain essential for keeping bacteria under control. Understanding how gum health impacts dental implants helps you maintain your results long-term.
You should visit your dentist every three to six months for checkups. These regular appointments allow your dental team to address any issues before they threaten your implant’s stability.