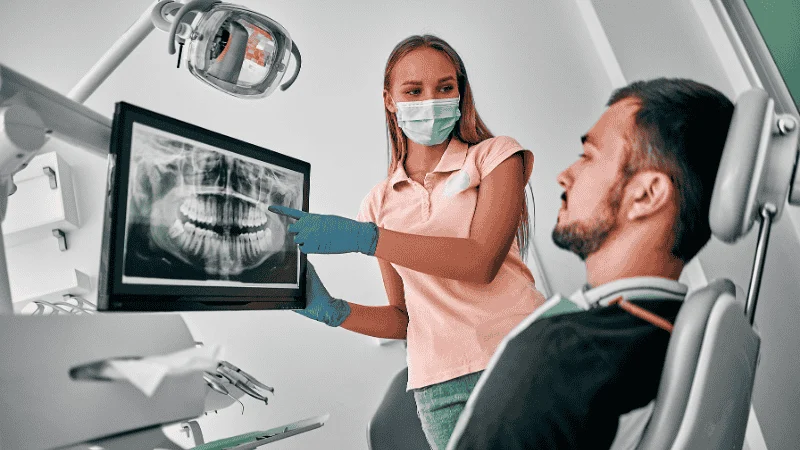
Dental implants have a high success rate, but they can fail. When that happens, you may feel pain, notice movement, or see swelling around the implant. Knowing why failure happens helps you protect your smile and avoid bigger problems.
Dental implant failure usually happens because of infection, poor bone support, too much pressure on the implant, or health and healing problems that stop the implant from bonding with your jaw.
Infection is one of the most common causes, often linked to poor oral hygiene or plaque buildup, as explained in this guide on dental implant failure signs and causes.
Other risks include smoking, uncontrolled diabetes, weak bone, surgical trauma, or excessive biting force.
You can also face problems months or years later. A condition called peri-implantitis, which involves inflammation and bone loss around the implant, plays a major role in late failure, as described in this review of peri-implantitis and implant failure causes.
When you understand these risks and warning signs, you take control of your long-term results.
Key Takeaways
- Dental implants fail due to infection, poor healing, excess force, or medical risks.
- Early signs include pain, swelling, mobility, and bone loss around the implant.
- Good hygiene, proper planning, and regular checkups lower your risk.
Receive advanced implant care across Miami, Pembroke Pines, and Delray Beach, FL today.
What Is Dental Implant Failure?
Dental implant failure happens when your implant does not stay stable or function the way it should. It can occur soon after surgery or years later, depending on the cause.
Definition and Stages
Dental implant failure means the implant does not properly bond with your jawbone or loses that bond over time. When this happens, the implant may feel loose, painful, or infected.
Dentists often divide failure into two stages:
- Early dental implant failure – This occurs before the implant fully fuses with the bone. It often shows up within the first few months. Problems during surgery, infection, or poor bone healing can lead to early implant failure.
- Late dental implant failure – This happens after the implant has healed and supported a crown. Late implant failure may develop years later due to bone loss, infection, or too much biting force.
You may notice swelling, discomfort, bleeding gums, or movement of the implant. A failed implant needs prompt care to prevent more bone loss.
Prevalence and Success Rates
Dental implants have a high dental implant success rate when placed and maintained properly. Many studies report strong long-term implant survival, especially in healthy patients who do not smoke and practice good oral hygiene.
Even so, failure can happen. According to a review on the etiology and management of dental implant failure, implant failure can result from both local and systemic factors, such as infection, poor bone quality, or uncontrolled medical conditions.
The overall implant failure rate is low compared to many other dental treatments. Still, your personal risk depends on your health, bone strength, and daily care habits. Regular dental visits help protect your implant success rate over time.
Types of Implant Failures
Dentists classify implant failure in a few clear ways. The most common types include:
1. Biological failure
This involves infection or poor bone healing. A key cause is peri-implantitis, a gum infection around the implant that leads to bone loss.
2. Mechanical failure
This includes broken screws, loose parts, or a fractured implant. Excess pressure from grinding or poor bite alignment can cause these problems.
3. Early vs. Late failure
Early dental implant failure happens before full healing. Late dental implant failure develops after the implant has already been in use.
Knowing the type of implant failure helps your dentist choose the right treatment and protect your remaining bone.
Visit our clinic to address dental implant failure causes early.
Major Causes of Dental Implant Failure
Dental implants fail when the bone does not bond to the implant, when infection damages the tissue, or when your health limits healing. These problems affect implant osseointegration, bone support, and long‑term implant longevity.

Poor Osseointegration
Osseointegration means your jawbone grows and bonds tightly to the implant. If this bond does not form, the implant becomes loose and may fail early.
Early failure often links to surgical trauma, overheating of bone, or movement of the implant during healing. Even small shifts can stop proper implant osseointegration.
Smoking, uncontrolled diabetes, and poor oral care also raise the risk. Some cases relate to immune response or poor bone quality. You may notice mobility before your final crown is placed.
To lower your risk, follow post‑surgery instructions closely. Avoid pressure on the implant and keep the area clean.
Peri-Implantitis and Infection
Infection is one of the most common causes of dental implant failure. Bacteria can build up around the implant and inflame the gum tissue.
This condition, called peri-implantitis, leads to bone loss around the implant. It often starts as mild inflammation and then worsens if you do not treat it.
Signs include bleeding gums, swelling, pain, pus, or a bad taste. In advanced cases, the implant may feel loose. Infection can happen months or even years after placement.
If you have a history of periodontal disease, your risk increases. Regular cleanings in periodontics care and good home hygiene protect your implant from peri‑implant disease.
Insufficient Bone Density or Volume
Your implant needs enough strong bone to stay stable. If you have insufficient bone density or volume, the implant may not anchor well.
Low bone density often affects the upper jaw. Bone loss from missing teeth, trauma, or long‑term dentures can also reduce support.
In some cases, your dentist may suggest bone grafting before implant placement. A graft builds up the area so the implant has a solid base.
If you have osteoporosis, your bone may be weaker. Your dentist will review scans and medical history to decide if extra support is needed.
Systemic Health Conditions
Your overall health plays a direct role in healing. Conditions like uncontrolled diabetes slow tissue repair and raise infection risk.
Osteoporosis can reduce bone strength, which affects implant stability. Certain medications, such as steroids or drugs used for bone disease, may also interfere with healing.
Autoimmune disorders and immune suppression can disrupt normal implant osseointegration. Smoking further limits blood flow and delays recovery.
These systemic factors are widely recognized among the main causes of implant failure. Managing your health, quitting smoking, and keeping medical conditions stable improve your chances of long‑term implant longevity.
Before surgery, share your full medical history. Careful planning helps your dental team reduce risk and protect your investment.
Book a consultation to prevent dental implant failure and protect your smile.
Surgical and Prosthetic Complications
Problems during implant surgery or after implant restoration can lead to failure. Placement errors, mechanical stress, and the wrong implant type all raise risk when you do not control them well.
Implant Placement and Surgical Technique
Your outcome depends heavily on accurate implant placement and careful implant surgery. If the surgeon places the implant at the wrong angle or depth, you may face chewing problems, bone loss, or early failure.
Poor surgical technique can damage bone or reduce blood supply. Early failure often links to surgical trauma and poor bone quality.
Surgeon experience also matters. A clinician with limited training may misjudge bone width or height, especially in complex areas like the upper jaw.
Procedures such as sinus lift or ridge augmentation add more risk. If healing does not go well or the graft fails, the implant may not bond with bone.
Implant location plays a role too. Back teeth handle stronger biting forces, so poor positioning in molar areas can overload the implant.
Prosthetic Issues and Screw Loosening
Even if surgery goes well, problems can start during implant restoration. Mechanical stress can cause screw loosening, fractured components, or chipping of the crown.
These are common prosthetic complications in both fixed and removable teeth designs.
When screws loosen, the implant may feel unstable. You might notice movement, discomfort, or trouble chewing.
A poor prosthetic design can also overload the implant. If the crown is too tall or not aligned with your bite, extra force transfers to the bone.
Regular follow-up visits help detect these implant complications early. Tightening a loose screw or adjusting the bite can prevent more serious damage.
Implant Type and Material Reactions
Your implant type affects long-term survival. Shape, surface design, and connection style all influence how well the implant bonds with bone.
A recent retrospective analysis on factors affecting dental implant failure found that implant type and restoration type significantly influenced survival rates.
Some implant designs achieve better primary stability in soft bone. Others may not perform as well in certain implant locations.
Material reactions are rare but possible. Most implants use titanium, which is generally well tolerated, but poor integration can still occur if stability is weak at placement.
Choosing the right implant type for your bone quality, bite force, and restoration plan lowers your risk of mechanical and biological failure.
Mechanical Factors and Patient Habits
Daily forces and personal habits can weaken even a well-placed implant. Excess pressure, tobacco use, and poor cleaning often lead to dental implant complications such as implant mobility or a loose dental implant.

Biomechanical Overload and Bruxism
Your implant must handle the force of biting and chewing every day. When that force becomes too high, biomechanical overload can damage the bone that supports the implant.
Common causes of overload include:
- Teeth grinding (bruxism)
- Clenching during stress
- Poor bite alignment
- Long cantilever bridges
Bruxism places repeated pressure on the implant, especially at night. Over time, this stress can reduce implant stability and lead to implant mobility.
Primary stability, which is the tight fit of the implant at placement, plays a key role. If primary stability is weak, overload can cause early failure. Even years later, heavy biting forces can still cause bone loss.
If you grind your teeth, your dentist may suggest a night guard. This simple step helps protect the implant and may improve how long dental implants last.
You should also report any signs of a loose dental implant right away. Early care can prevent more damage.
Smoking and Tobacco Use
Smoking slows healing and reduces blood flow to your gums. This makes it harder for bone to attach firmly to the implant.
Research on the etiology and management of dental implant failure lists smoking as a major risk factor for both early and late failure. Smokers face higher rates of infection and bone loss around implants.
Tobacco also weakens your immune response. This raises your risk for peri-implantitis, an infection that can lead to implant mobility.
If you smoke, you increase the chance of dental implant complications such as:
- Delayed healing
- Bone loss
- Implant instability
- Higher failure rates
Quitting before and after surgery improves healing. Even cutting down can help, but stopping fully offers the most benefit.
Oral Hygiene Practices
You must clean around your implant every day. Plaque builds up just like it does on natural teeth.
Poor oral hygiene allows bacteria to grow along the gum line. This can cause inflammation and bone loss, which may reduce implant stability.
Signs of trouble include:
- Bleeding gums
- Swelling
- Bad taste
- Implant mobility
Peri-implantitis often begins without pain. Regular brushing with a soft brush and daily flossing help prevent it.
Professional cleanings are also important. Your dentist can check bone levels and make sure your implant remains stable.
Good home care plays a direct role in how long dental implants last. Consistent cleaning lowers your risk of serious dental implant complications.
Recognizing the Signs of Implant Failure
You can often spot early signs of dental implant failure if you know what to watch for. Pain, changes in your gums, and movement in the implant are clear warning signals that need quick attention.
Pain, Swelling, and Discomfort

Some soreness is normal right after surgery. It should improve within a few days to a couple of weeks.
If you feel persistent pain, throbbing, or pressure that does not fade, your implant may not be healing as it should. Ongoing swelling, tenderness, or pus around the implant site can point to infection.
Infection around an implant is often called peri-implantitis. It can damage the bone that supports your implant.
Pay attention to pain when you bite or chew. Sharp or increasing discomfort is not normal months after placement. Call your dentist if pain lasts, gets worse, or returns after healing.
Gum Recession and Inflammation
Healthy gums should fit snugly around your implant. They should look pink and feel firm.
If you notice gum recession, where the gum pulls back and exposes part of the implant post, this can signal a problem. Gum recession often happens when infection or bone loss develops under the surface.
You may also see redness, swelling, or bleeding when you brush. These are common signs of dental implant failure linked to inflammation. Poor oral hygiene and untreated gum disease increase this risk.
This overview of dental implant failure causes and symptoms explains how infection and bone loss affect the tissue around an implant.
Do not ignore small changes in your gums. Early treatment can stop further damage and may save your implant.
Implant Looseness and Mobility
A successful implant should feel stable, like a natural tooth. It should not shift when you touch it with your tongue or press on it gently.
If your implant feels loose, moves when you chew, or clicks under pressure, you may have a failed dental implant. This often means the implant did not bond fully with your jawbone, a process called osseointegration.
Bone loss from infection or excess bite force can also cause movement. Teeth grinding and uneven bite pressure place extra stress on the implant.
Implant movement is never normal. Contact your dentist right away to prevent further bone damage.
How to Prevent Dental Implant Failure
You can prevent dental implant failure by choosing the right patient, using careful surgical methods, and committing to long-term care. Each step protects bone health, lowers infection risk, and supports a strong implant success rate.
Patient Assessment and Risk Factor Management
You need a full health review before implant surgery. Your dentist should check for uncontrolled diabetes, smoking, gum disease, and bone loss, since these risk factors raise the chance of early or late failure.
Poor bone quality and untreated infection often lead to problems, as explained in this review on the etiology and management of dental implant failure. When you control medical issues and treat gum disease first, you improve healing.
Your provider should also:
- Take detailed X-rays or 3D scans
- Measure bone height and width
- Review medications like steroids or bisphosphonates
- Discuss teeth grinding or clenching
If you smoke, quitting before surgery can lower your risk. If you grind your teeth, you may need a night guard. These steps directly support implant stability and reduce the need for implant removal or re-implantation later.
Optimizing Surgical Techniques
Surgical precision plays a major role in how to prevent dental implant failure. Your surgeon must place the implant in the correct position and angle to spread bite forces evenly.
Overheating the bone during drilling or failing to secure strong initial stability can lead to early failure.
To lower risk, your surgeon should:
- Use proper cooling during drilling
- Avoid placing implants in active infection
- Ensure firm primary stability
- Design the crown to prevent overload
Accurate planning reduces stress on the implant. When bite forces stay within safe limits, you protect the bone and support long-term success.
Long-Term Aftercare and Maintenance
Your daily habits matter as much as the surgery. Plaque buildup can cause peri-implantitis, an infection that damages bone around the implant.
Brush twice a day and clean around the implant with floss or special brushes. Regular dental visits allow your dentist to check for:
- Bleeding around the implant
- Deep pockets
- Bone loss on X-rays
- Loose screws or parts
If your dentist finds a problem early, treatment may stop bone loss and prevent implant removal. Consistent care protects your investment and keeps your implant strong for years.
Frequently Asked Questions
Dental implant failure usually ties back to infection, poor bone support, or too much pressure on the implant. You may notice pain, movement, or swelling before the implant fully fails, and long-term problems can show up years later.
What are the three major reasons for failure of implants?
The three main causes are infection, failure to bond with the bone, and excessive force on the implant.
Infection around the implant, often called peri-implantitis, can damage the gum and bone.
Poor bone integration can happen if you have low bone density, uncontrolled diabetes, or if the implant lacks stability at placement. Excess pressure from teeth grinding or a poorly designed crown can also overload the implant and cause it to loosen.
Who is typically responsible when a dental implant fails?
Responsibility depends on the cause. If the failure results from surgical errors or poor planning, your dentist or surgeon may be accountable.
If you smoke, skip cleanings, or ignore care instructions, those factors may contribute to the problem. Some failures happen even when both you and your provider do everything right, especially if you have health issues that affect healing.
What are some early signs that a dental implant may not be successful?
Early warning signs include movement, pain when chewing, swelling, or pus around the implant. Bleeding gums and ongoing discomfort are also red flags.
Early failure often happens because of infection at the implant site or problems during healing. If you notice any of these signs, contact your dentist right away.
How common is it for dental implants to fail, and why?
Dental implants fail in about 2% to 5% of cases. Most failures link to smoking, uncontrolled diabetes, infection, or heavy bite pressure. Good planning and regular checkups lower your risk.
Can a dental implant fail after 10 years, and what might cause that?
Yes, an implant can fail even after 10 years. Late failure often results from bone loss around the implant or long-term infection.
Ongoing stress from grinding your teeth or a loose screw can also weaken the structure over time. Research shows that mechanical issues, like screw loosening, increase over many years of use, which raises the risk of complications.
Are there any refunds or compensation options for a failed dental implant?
Refunds depend on your dental office policy and any written treatment agreement you signed. Some offices offer partial refunds or free replacement within a set time frame.
Dental insurance may cover part of the cost to remove or replace a failed implant, but coverage varies. If you believe negligence played a role, you can request your records and seek a second opinion before taking further steps.